You can now export your own PREP-C data
Mon, Jul 16th 2018, 16:04
On the top of your 'Portal' just click on 'Reports'

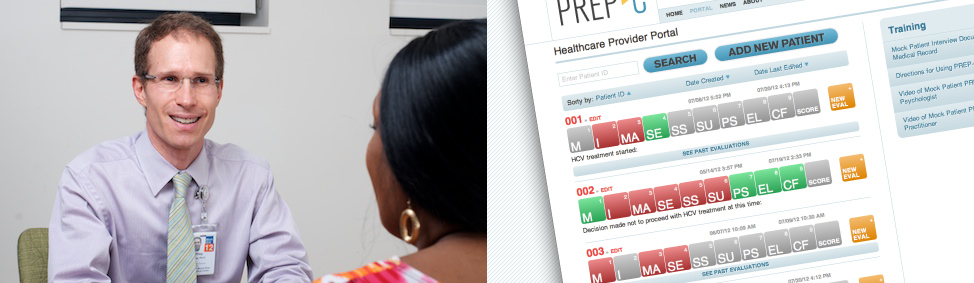
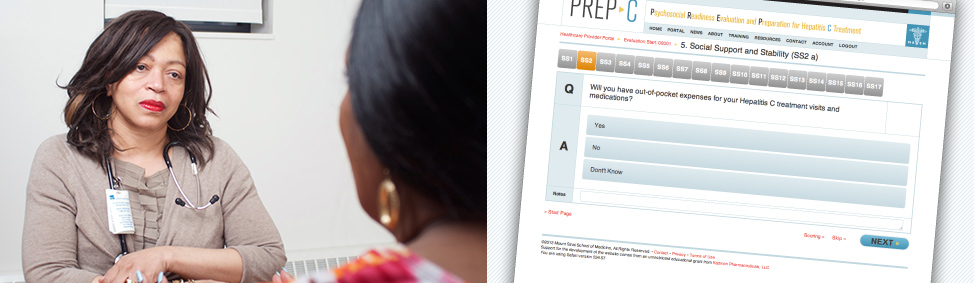
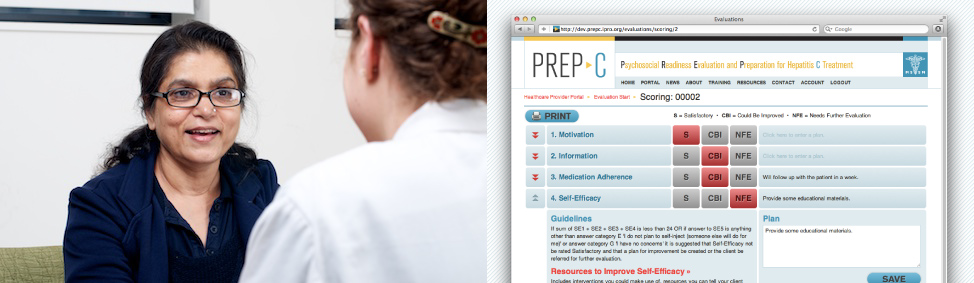

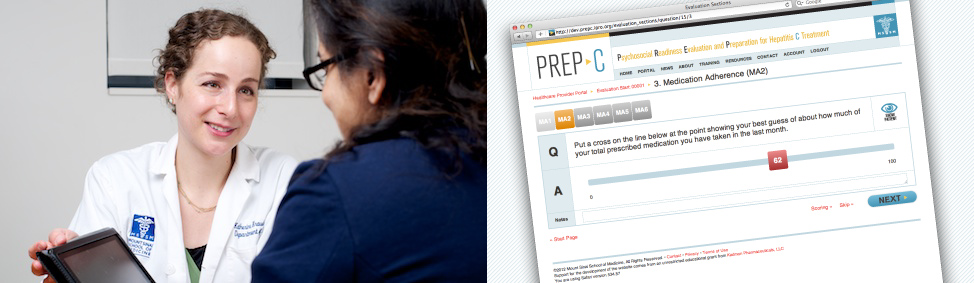

The Psychosocial Readiness Evaluation and Preparation for Hepatitis C Treatment (PREP-C) is a free interactive online tool that enables you to provide a thorough assessment of a patient’s psychosocial readiness to begin Hepatitis C treatment, and make a treatment plan to improve treatment readiness.
This free online tool can be used by any type of professional involved in preparing a patient for Hepatitis C Treatment including medical providers, nurses, mental health, substance use, social work, pharmacy, case management, treatment adherence and health education specialists.
We invite you to learn more about the PREP-C in the About and Training sections. We hope that after doing so you will Register as a user and begin to use the PREP-C to help your patients prepare to start Hepatitis C treatment.
Mon, Jul 16th 2018, 16:04
On the top of your 'Portal' just click on 'Reports'
Confidentiality
Registration for the PREP- C is quick, easy & free.
In order to register, you will need to enter basic information about your professional role, and read and agree to the web site’s Terms of Use and Privacy Policy.
What you can expect from the PREP-C